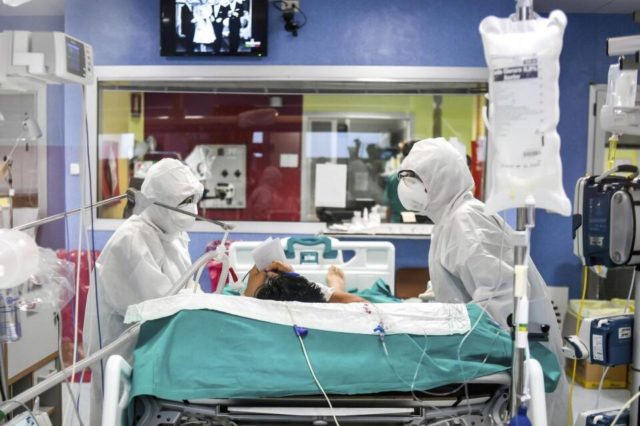
Currently there are only two operational state-managed intensive care units in the entire Northern Cape – one in Kimberley and the other one in Upington.
THERE are currently only two operational state-managed intensive care units in the entire Northern Cape, one at the Robert Mangaliso Sobukwe Hospital in Kimberley and the other at the Dr Harry Surtie Hospital in Upington.
According to DA provincial leader Andrew Louw, this was revealed by the MEC for Health, Maruping Lekwene, during a virtual health portfolio committee meeting on Tuesday.
The DA in the Northern Cape has called on the provincial Health Department to prioritise the operationalisation of additional intensive care units across the Province.
Louw said that the fact that there were only two intensive care units (ICU) in the Province was “very worrying”. “This means that there is an expanse of hundreds of square kilometres of the Province without quick access to lifesaving ICU facilities.”
According to Louw, people residing in the far end of Namaqualand would have to be transported to Upington, or even to Kimberley, for emergency care, while those in De Aar and surrounds would have to be transported to Kimberley.
“This is in spite of the new, multimillion-rand hospital that was not so long ago opened in De Aar. This is ironic, given that the Pixley ka Seme District, in which De Aar falls, is the very district that has been used to pilot the National Health Insurance (NHI) plan; simply proving once again that the NHI is not the answer to the Province’s many health challenges.”
Louw pointed out that the Northern Cape also has a very poorly capacitated emergency medical service (EMS), which currently only has about 80 operational ambulances servicing the entire Province, and which is increasingly relied upon for referrals from the districts to the better equipped facilities.
“This is a growing crisis at any given time, even more so now as the Province finds itself in the eye of the (Covid-19) pandemic, with more people likely to require intensive care and ventilation.”
The DA called on Lekwene to prioritise not only the capacitation of De Aar Hospital, but also at least one hospital in the John Taolo Gaetsewe District and one in Namaqualand. “At the very least, each district should have a well-resourced and professionally staffed hospital, able to provide high-level medical care as opposed to mere clinic-type health care services.
“It is undeniable that Covid-19 has exposed deep-seated flaws in the provincial health system and that if urgent reform of existing facilities is not prioritised, we will see more and more people dying, not only from Covid-19 complications necessitating ventilation in ICU, but also of cases of maternal and neo-mortality, motor-vehicle accidents, cardiovascular conditions, strokes and the many other health-related conditions that require intensive care,” Louw said..
The MEC of Health in the Province, Maruping Lekwene, said during a media briefing last week that the Northern Cape was ready for the anticipated Covid-19 peak in the Province, which was expected towards the middle to the end of September.
According to Maruping, the Province currently has almost 3 000 beds ready and was working on increasing that number to 4 000 beds.
He stated further that there were 65 Intensive Care Unit (ICU) beds ready while the department was currently busy connecting an oxygen supply to those beds.
He also gave the assurance that there were enough ventilators in the Province.
“It is vital that there is enough oxygen and sufficient ventilators which will help save lives, so we are working on increasing our oxygen capacity. We are also looking at equipping the new De Aar hospital, as well as other clinics and hospitals in the Province, in order for them to assist people who may need hospitalisation when the peak hits the Northern Cape.”
“As a Province, we want to ensure that we have adequate equipment and manpower to assist our people should the worst happen,” he said, adding that preparations had been made to increase the manpower, with an additional 160 nurses employed and 30 additional doctors as well as increased staff in other fields.